THE WORLD'S FIRST PAIN MANAGEMENT FOCUSED AI MODEL
Get Paid on Every Claim
Ensure higher first-time approvals for prior auths and claims — while staying payer-compliant — with Mainer, developed by PainMedPa
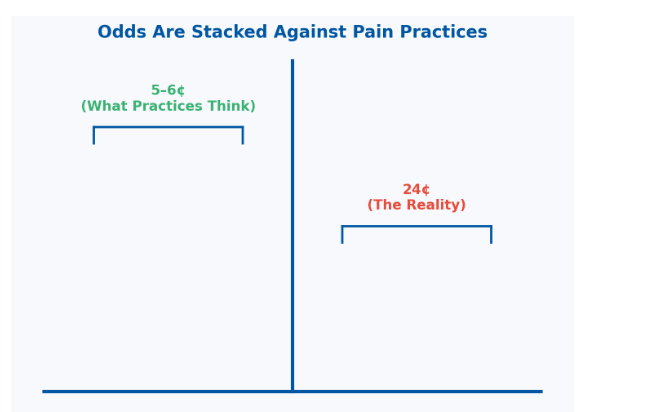
Odds Are Stacked Against Pain Practices
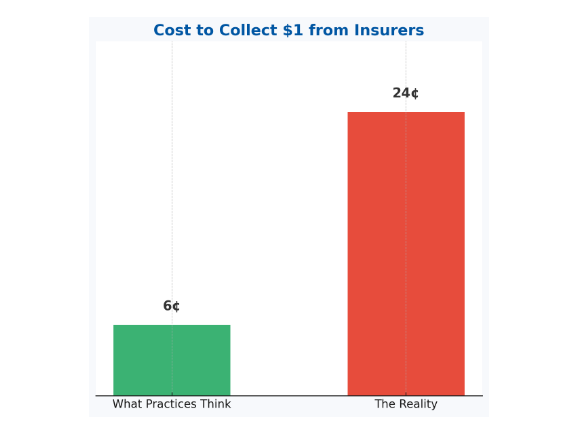
Most practices think they spend 5–6¢ to collect a dollar. The reality? They're losing 20¢ on every dollar without realizing it.
Lost on Every Dollar
Hidden costs from denials, delays, and unpaid claims
Dropping Approval Rates
First-time approvals declining across all payers
Why Pain Practices Are Bleeding Money
Moving Goalposts
Payer guidelines shift constantly. What was approved yesterday gets denied tomorrow.
Complex Documentation
Charting requirements multiply while still falling short of payer expectations.
Revenue Leakage
More rework, more delays, more money left on the table.
What Sets Mainer Apart
The first AI built exclusively for Pain Management practices. Trained on 100,000+ real encounters to deliver specialty-specific intelligence.
Specialty-Specific AI
Not generic healthcare AI. Built specifically for Pain Management practices with deep understanding of your specialty's unique challenges.
Proven Results
Real metrics from practices already using Mainer: 30% fewer denials, faster approvals, significant cost reductions.
Auto-Compliance
Automatically updates with payer and Medicare rule changes, keeping you compliant without manual effort.
Real Results from Real Practices
See the measurable impact Mainer delivers
Fewer Denials
Reduction in claim rejections across all payers
Faster Approvals
Prior authorizations processed in hours, not days
Compliance Updates
Automatic updates on payer and Medicare rules
Why We Built Mainer: Giving Pain Practices Their 20¢ Back
Pain practices lose as much as 20¢ on every $1 collected. We built Mainer to give that back.
Fight AI with AI
Payers are already using algorithms to review documentation, downgrade visits, and deny claims.
Mainer ingests payer-specific guidelines and guides providers on proper documentation so your charts stand up to insurer AI.
Reduce True Cost of Collections
Billing isn't about staff expense—it's about revenue lost to denials and errors.
Mainer automates billing, improves first-time approvals, and ensures every claim gets paid in full and on time.
Recover Lost Revenue
Get back the money you're losing to denials and delays
Faster Approvals
Higher first-time approval rates for prior auths and claims
Stay Compliant
Auto-updates on payer and Medicare rule changes
Ready to Stop Losing 20¢ on Every Dollar?
With Mainer, powered by PainmedPa, the money stays where it belongs—in your practice.
Get Started TodayOne Rate. Everything Included.
No hidden fees, no surprise charges. Just one transparent rate that covers everything you need.
Covers everything you need
Prior Authorization
Complete prior auth management and submission
Billing Services
Full billing and claims processing
Compliance Support
Documentation and compliance guidance
EMR Compatibility
On another EMR? Contact us for tailored pricing.
Save More Than You Spend
While you pay 3.75% for our services, you'll recover the 20¢ you're currently losing on every dollar collected.
Not just new tech. Built on PainmedPa's track record.
PainmedPa is already trusted by Pain Management practices nationwide.
Contact Our Team
contact@painmedpa.com
AI built for Pain Practices — fewer denials, faster approvals, compliant by design.